Clinical quality management Hedis/Stars
Together, we will do this
Fuel your quality program with EXL Health Quality ratings and the financial health of a health plan are intertwined and it’s becoming imperative for health plans and providers to bolster their quality programs with intelligence. Measures and reporting requirements become more complex every year; health plans and providers are working harder than ever to achieve the coveted five-star rating for their services which improves outcomes and revenue. It is important to gather and analyze information in a timely manner. EXL Health provides a holistic solution to give payers and providers the insights they need to deliver better quality of care, drive member engagement and performance measurement.
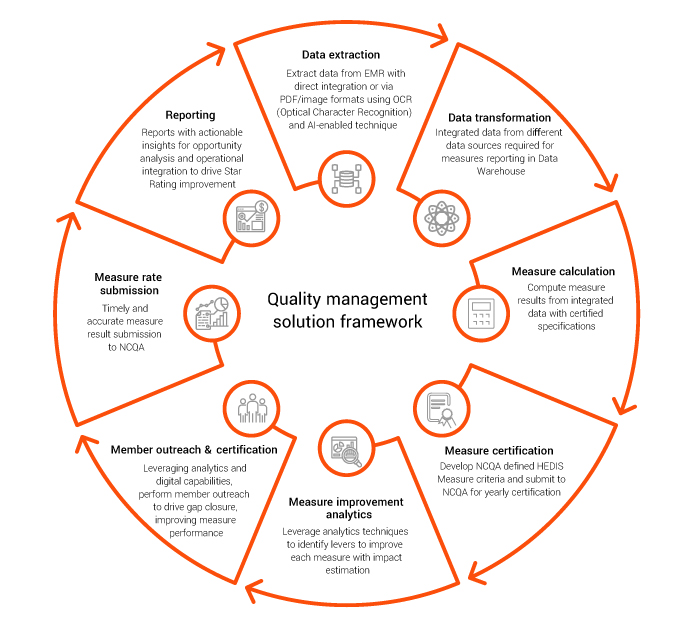
End-to-end quality management solution EXL Health’s modular, end-to-end solution is a combination of products and services to drive improvements across your quality management ecosystem. Our solution enables you to integrate data from different departments and platforms into a single, cohesive process that covers HEDIS, Stars, HEDIS-like, and other required measures. Combined with our robust analytics, these can be integrated into any existing workflow to drive member engagement for each measure. Leveraging EXL’s quality management solution, health plans can:
- Seamlessly integrate all data sources.
- Identify high risk members for proactive outreach.
- Close member care gaps by addressing their barriers to care and noncompliance.
- Comply with HEDIS reporting requirements and improve Star ratings.
- Deliver an engaging member experience.
- Improve patient outcomes & drive compliance.
Leverage EXL’s deep domain expertise in healthcare, data, and analytics to measure performance and drive proactive improvement
Our solution provides end-to-end support to inform strategy, improve quality of care, and improve ratings.
Core components of the solution include:
- Medical chart retrieval.
- NLP algorithms that extract and abstract information to support condition identification, and gaps in care.
- Complex structured and unstructured data source integration with comprehensive Member 360° analytics.
- Aggregate and harness data to drill down from a provider to a member and all the way to a claim level.
- Certified HEDIS, Stars and other quality measures critical to manage population risk.
- Workflow integration for ease of use by physicians, nurses and coders.
- Reporting and analytics to deliver insights and drive operations through smart integration.
- Predictive analytics by measure set to drive engagement and outreach.
- Tailored messages delivered in a multi-channel communication framework.
- Process and submit to NCQA for certification and approval.
Empowered with EXL’s smart, data-driven predictive model output, healthcare providers can proactively engage with members to drive better quality of care, boost Star ratings, and enhance member experience. Prepopulated and customizable scorecards and dashboards deliver prescriptive and actionable insights.
Why EXL Health?
EXL Health delivers an end-to-end quality management solution. From expert clinical knowledge, data extraction and warehousing to advanced analytics, we give the analysis and tools needed to make the maximum impact on Quality management initiatives. Our client-first approach leverages on strong domain expertise, technology and services spanning clinical, operational and financial areas to deliver right-size offerings. URAC and NCQA accredited, we combine enterprise data management, real-time analytics, and innovative approach required to solve real-world problems.
